Hiatal hernia
What is diaphragmatic hernia and how is it treated?
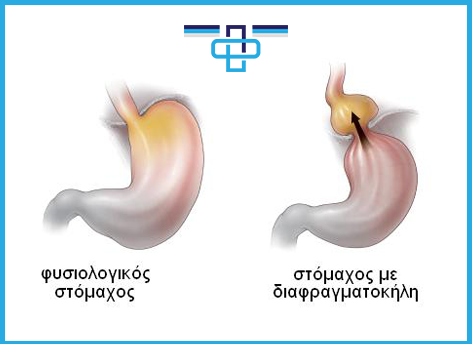
A hiatal hernia is an uncommon form of internal hernia (it occurs inside the abdominal cavity), resulting by protrusion of the stomach into the thorax. A small hiatal hernia is almost always asymptomatic, and it is usually discovered incidentally during routine gastroscopy. However, as the hernia enlarges progressively, mild to severe symptoms may encounter.
Most people with hiatal hernia don’t experience any symptoms by the hernia itself, but as a result of the accompanying acid reflux to the esophagus, which may lead to:
- Indigestion / bloating
- Dysphagia
- Retrosternal pain (“burning”)
- Hiccups
Long standing gastroesophageal reflux due to the presence of a hiatal hernia may alter the normal anatomy of the lower esophagus (metaplasia / dysplasia), which in some cases may lead to the development of esophageal carcinoma. Except for acid reflux, other problems related to this type of hernia are strangulation and bleeding due to erosion of the stomach blocked inside the hernia.
The symptoms of the co-existent gastroesophageal reflux are usually improved by conservative means, such as:
- Weight loss
- Eating small and frequent meals
- High-protein and low-fat diet
- Avoidance of food consumption 3-4 hours before sleep
- Anti-acid medication (PPIs)
However, most of cases of hiatal hernias require surgical treatment. The repair of the hernia is carried out laparoscopically by reducing the stomach inside the abdomen and by suturing the diaphragmatic crura. In most cases, due to the coexistence of gastroesophageal reflux, an anti-reflux procedure is also performed. This is done by wrapping the fundus of the stomach around the lower part of the esophagus (laparoscopic fundoplication). The hospital stay after the procedure is short, and the patient returns quickly to his every-day activities, with specific dietary instructions for a short period of time.